Literature & Publications
|
This article originally appeared in the July issue of Irish Dentist. Reprint approved by the Irish Dentist editorial board. |
||
|
||
|
KEN KEATING GIVES AN ENGINEER'S PERSPECTIVE ON TWO METHODS OF CONNECTING AN ABUTMENT TO AN IMPLANT |
||
| Osseointegrated implants are one of the fastest growing dental treatments in Ireland today. They are not new, implant restorations have been in use for over 30 years now. They are used singularly as replacement for single tooth loss and as the support for a bridge either to a natural tooth or to another implant. Multiple implants are also used to support prostheses, e.g. full or partial dentures. An implant is a mechanical system designed to transmit occlusal forces on a prosthesis through an abutment and implant to the surrounding bone. In the United States alone, there are more than 50 companies involved in manufacture or marketing of dental implants. Brunski (1999) states that implant design is driven by copying and modifying existing designs rather than fundamental advances in biomechanics. The original and most copied method of attaching the abutment to the implant is by means of a screw. It is still the method common to most implant systems. Screw loosening and screw breakage is a major disadvantage of this method. Jemt et al (1991) have shown that screw loosening appears to be a bigger problem with single tooth restorations. There is an alternative to screw retained abutment systems; a Boston based implant company called Bicon uses a locking taper system to connect the abutment. In this article, I will give an engineers perspective on these two methods of connecting the abutment to the implant. | Ken is a mechanical engineer and is a member of the academic staff of the Dublin Institute of Technology, Department of Engineering Technology, since 1994. He is engaged in research and is supervising several student projects on dental implants. He is currently carrying out comparative studies on methods of attaching abutments to oral implants. Ken recently delivered a presentation at the Irish Dental Association’s Scientific Conference in Kilkenny | |
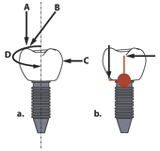 Figure 1a: Forces Figure 1b: Moments |
FORCES ON SINGLE IMPLANTS To an engineer the mastication forces on an implant can be analysed as a statically equivalent system of forces and moments. The forces acting on the prosthesis are shown in Figure 1a. They can be, a. vertical forces, usually acting eccentric to the central axis, b. inclined forces that resolve into a vertical and horizontal component, c. lateral forces, and d. torsional forces. It is important to note that these forces vary in intensity with location in the mouth and are often cyclical in action. Vertical forces tend to be larger in the posterior than in the anterior regions. The maximum vertical biting force in humans was found by van Eijden (1991) to approach 800N, and Graf (1975) estimates the lateral forces to be in the order of 20N. Furthermore, lateral components of inclined forces in the incisal region can be appreciable (Brunski 1999). In the case of screwed abutments, these forces produce moments, about the screw joint (see Figure 1b). Vertical forces act about the centreline of the implant. Horizontal or lateral forces act about the plane of the abutment/implant interface. The combined effect is to continually subject the implant restoration to joint-separating forces of a magnitude greater than the mastication forces. |
|
| SCREW PRELOAD Preload, shown in Figure 2, is the axial force in the neck of the screw, which is between the first mating thread and the head of the screw. This tensile force clamps the abutment to the implant. The importance of preload cannot be overestimated. It improves both the locking effect and the fatigue strength of the screw. To be effective the level of preload must be less than the elastic limit or proof load, i.e. the maximum load at which no permanent deformation occurs, of the screw material and greater than any force applied by biting action. Depending on the stiffness of the screw material and whether or not the screw is being reused, preloads of 75% to 90% of the material elastic limit may be required to prevent loosening under moderate lateral loads. For ductile materials such as commercially pure titanium or gold, this gives very little room for error. Is this degree of accuracy attainable? Burguete et al (1994) found torque wrenches to be of limited value for tightening gold screws. They showed that a 25% variation in applied torque resulted in a 66% variation in preload. On top of this, Shigley and Mischke (1986) state that 10% of preload is lost to embedment relaxation. Junker and Wallace measured errors of between 23% and 28% in hand torque wrenches, and errors of between 17% and 23% in power torque wrenches. Why is it so difficult to achieve optimum preload on a screw-retained abutment? The relationship between applied torque and preload depends on several factors. They include: • Screw geometry • Material properties, particularly stiffness • Surface texture and condition of the mating surfaces • Degree of lubrication • Rate of tightening • Integrity of joint (see Figure 3). This is why engineers measure strain (percentage change in length of bolt), not torque when pre-load tolerances are narrow. Critical components on your car such as the driveshaft bolt or the cylinder head bolts are lightly torqued and then angle tightened i.e. the bolt is turned through a predetermined angle that ensures preload is close to optimum value. In engineering, single screw threads are never used for clamping purposes, and locking devices and/or thread adhesive is usually used. |
 Figure 3: Screw joint showing gaps |
|
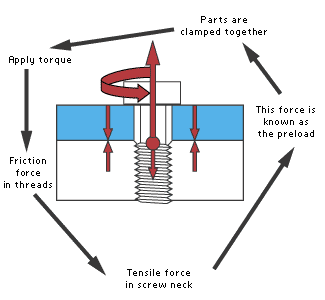 Figure 2: How torque develops preload |
||
| FRICTION The force that keeps a screw tight is the friction force between the threads, the head of the bolt and the abutment, and the implant and the abutment. The value of the friction force depends on the preload as well as the material combination, the surface texture, and the degree of contamination or lubrication. At a micro level friction is the interlocking and welding together of minute peeks called asperity on the opposing surfaces. If any movement, even micromovement occurs parallel to the plane of friction then the asperity are sheared off and produce an abrasive powder between the two surfaces (see Figure 4). Hamrock, Jacobson and Schmid (1999) state that the volume removed by wear is inversely proportional to the hardness of the materials; this implies that titanium alloys wear less than pure titanium. The preload forces the surfaces to close the minute gaps. This leads to a reduction in preload and friction force thus reducing the rigidity of the assembly making it more prone to lateral loads and so the cycle continues. Once this cycle begins it inevitably leads to the screw loosening eventually. The reduction in rigidity may also cause the screw to bend and even break due to fatigue wear. |
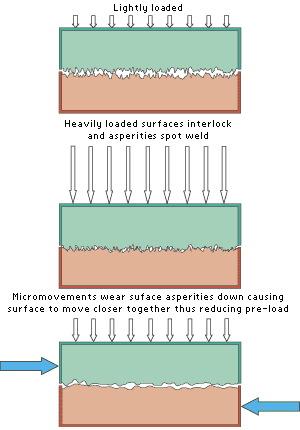 Figure 4: Shows how preload is lost as asperity break off due to lateral movement |
|
| LOCKING TAPER ABUTMENT The Bicon locking taper abutment has no screw, but like a screw-retained abutment, it relies on friction to keep it intact. Assembly is achieved by driving the 1.5 degree morse taper into the matching socket in the implant. A high clamping force between abutment and implant is generated by this action. The difference, shown in Figure 5, is that this clamping force is almost lateral to the axis of the implant and therefore almost normal or perpendicular to the friction plane. This means that lateral forces and moments about the abutment do not tend to wear down the surface asperity This is also improved by the use of Ti-6Al-4V titanium alloy, which is considerably stronger and stiffer than commercially pure titanium, and cold welds better, particularly in the absence of oxygen (Buckley, 1981). The high friction force is the result of relative slip between the two friction surfaces occurring at high contact pressure. This results in the surface oxide layers breaking down and the asperity fusing, sometimes referred to as cold welding. Therefore, as shown in Figure 6, there are no gaps between the abutment and the implant, unlike screw assemblies. Locking taper assemblies are rigid and can withstand high compressive axial forces and lateral forces without loosening. Because of the high friction force, they will resist pullout forces unless accompanied with torque to break the fused asperity Because of this, locking tapers are widely used in engineering wherever high axial and/or lateral loads with or without vibration are encountered. This ranges from machine tools, pulleys and bearings, up to propellers on bulk carriers. |
||
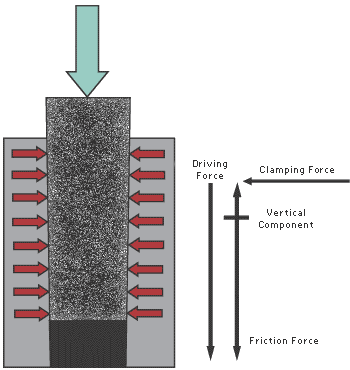 Figure 5: Retaining forces in locking taper abutments |
||
 Figure 6: Shows interface between Bicon locking taper abutment and implant |
||
|
CONCLUSION A high percentage of screws in single implant abutments come loose necessitating several retightening sessions. The equipment available for tightening screws is inadequate for the task demanded by virtue of the many variables encountered and tight tolerances required. The forces, fit, material properties and service conditions, all work against the screw retained abutments, but these same factors work for the locking taper abutments. |
||
|
REFERENCES Brunski JB (1999). In vivo bone response to biomechanical loading at the bone/dentalimplant interface. Adv Dent Res 13: 99-119 Buckley DH (1981). Surface effects in adhesion, friction, wear, and lubrication. Elsevier, New York Burguete RL et al (1994). Tightening characteristics for screwed joints in osseointegrated dental implants. J Prosthet Dent 71: 592-9 Graf H (1975). Occlusal forces during function. In: Rowe NH, ed. Occlusion: research on form and function. University of Michigan, Ann Arbor 90-11 Hamrock BJ, Jacobson B, Schmid SR (1999). Fundamentals of machine elements. McGraw- Hill, New York Jemt T, Lacey WR, Harris D, et al (1991). Osseointegrated implants for single tooth replacement: A 1-year report from a multicenter prospective study. Internatinal Journal Oral Maxillofac 6: 29 Junker GH, Wallace PW (1984). The bolted joint: economy of design through improved analysis and assembly methods. Proc Instn Mech Engrs 198B: 255-66 Shigley JE, Mischke CR (1986). Standard handbook of machine design. McGraw- Hill, New York Van Eijden (1991). Threedimensional analysis of human bite-force magnitude and moment. Arch Oral Biol 36: 535-539. |
||